Removal of condylomas - Condylomas (HPV)
Condylomas (genital warts) result from HPV infection and are among the most common sexually transmitted diseases. At Palmotićeva Clinic we remove condylomas using electrocautery, cryotherapy and chemical ablation, with complete HPV typing to assess the risk of cervical dysplasia.
What are condylomas (genital warts)?
Condylomas (condylomata acuminata) are one of the most common sexually transmitted diseases. These genital warts appear as small, cauliflower-like bumps — they can range from one millimeter to considerably larger formations. They are caused by the human papillomavirus (HPV).
There are over 100 types of HPV, but only a few highly contagious types cause condylomas. The virus is transmitted through sexual contact with an infected person — it is estimated that 2 out of 3 people who had contact with an infected individual will develop condylomas. They usually appear within the first 3 months but can also manifest after several years.
Symptoms of condylomas
The most common signs and symptoms include:
- Visible warts in the genital area — in women, they appear on the labia majora and minora, at the vaginal entrance, and less commonly inside the vagina and on the cervix
- In men — they appear on the penis (on the foreskin, urethral opening, or base of the penis)
- Anal location — they may appear around the anus or in the mouth and throat after oral sex
- Burning sensation or itching in the genital area
- Asymptomatic course — condylomas often cause no symptoms at all
When to see a doctor?
You should visit a gynecologist or urologist if:
- You notice condylomas in the genital area
- Your partner has condylomas
- You notice any unusual growths or skin changes on your genitalia
Genital warts can indicate a serious health problem — HPV is linked to cervical cancer, as well as cancers of the vagina, anus, and penis. Although the HPV types that most commonly cause condylomas usually do not cause cancer, simultaneous infection with multiple virus types is possible.
Treatment methods for condylomas
Some condylomas are not visible to the naked eye — in such cases, the doctor uses acetic acid to highlight them and a colposcope to locate them. It is important to note that removing the warts does not eliminate the virus itself, so recurrence is possible even after treatment.
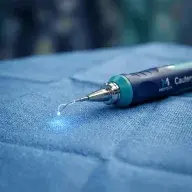
- Electrocauterization — removal of warts using an electrosurgical knife
- Cryotherapy — freezing condylomas with liquid nitrogen; during healing, blisters along with the condylomas fall off and new skin appears
- Laser therapy — uses a light beam to remove multiple lesions; a more expensive method with potentially slower wound healing
- Surgical excision — cutting out the warts surgically under local anesthesia
- Topical treatments — most commonly based on Podophyllin or trichloroacetic acid (TCA)
Protection and prevention
HPV can be transmitted from any part of the infected skin. Condom use significantly reduces the risk of transmission. Key preventive measures include:
- Regular gynecological examinations and Pap smear — enable early detection of changes in the vagina or cervix caused by the virus
- More frequent check-ups — after having had condylomas, a Pap smear every 6 months is recommended
- Vaccination (Gardasil) — protects against the most dangerous HPV types; the vaccine is available at our clinic
- Avoiding sexual intercourse until condylomas are treated — whether in yourself or your partner

Performed by
Dr Slobodanka Petković
Specialist in Gynaecology & Obstetrics · 35+ years of experience
Patients often ask
Condylomas are benign wart-like growths on the skin and mucous membranes of the genital area caused by human papillomavirus (HPV), most commonly types 6 and 11. They are transmitted through direct skin contact during sexual intercourse. Incubation lasts from 3 weeks to 8 months.
At our clinic we use electrocautery (removal with electric current), cryotherapy (freezing with liquid nitrogen) and chemical ablation. The choice of method depends on the location, number and size of condylomas. The procedure is performed on an outpatient basis with local anaesthesia.
Yes, recurrence is possible in 20–30% of cases because the virus can remain latent in surrounding tissue. Regular check-ups at 3–6 month intervals after removal are important. Strengthening the immune system reduces recurrence risk.
The HPV types that cause condylomas (6 and 11) are low-risk and rarely lead to cancer. High-risk types (16, 18, 31, 33...) can cause dysplasia and cervical carcinoma. This is why HPV typing is crucial for risk assessment.
Yes, partner examination and treatment is recommended as HPV is transmitted through contact. Condom use reduces but does not eliminate the risk of transmission, as the virus can be present on surrounding skin not covered by the condom.