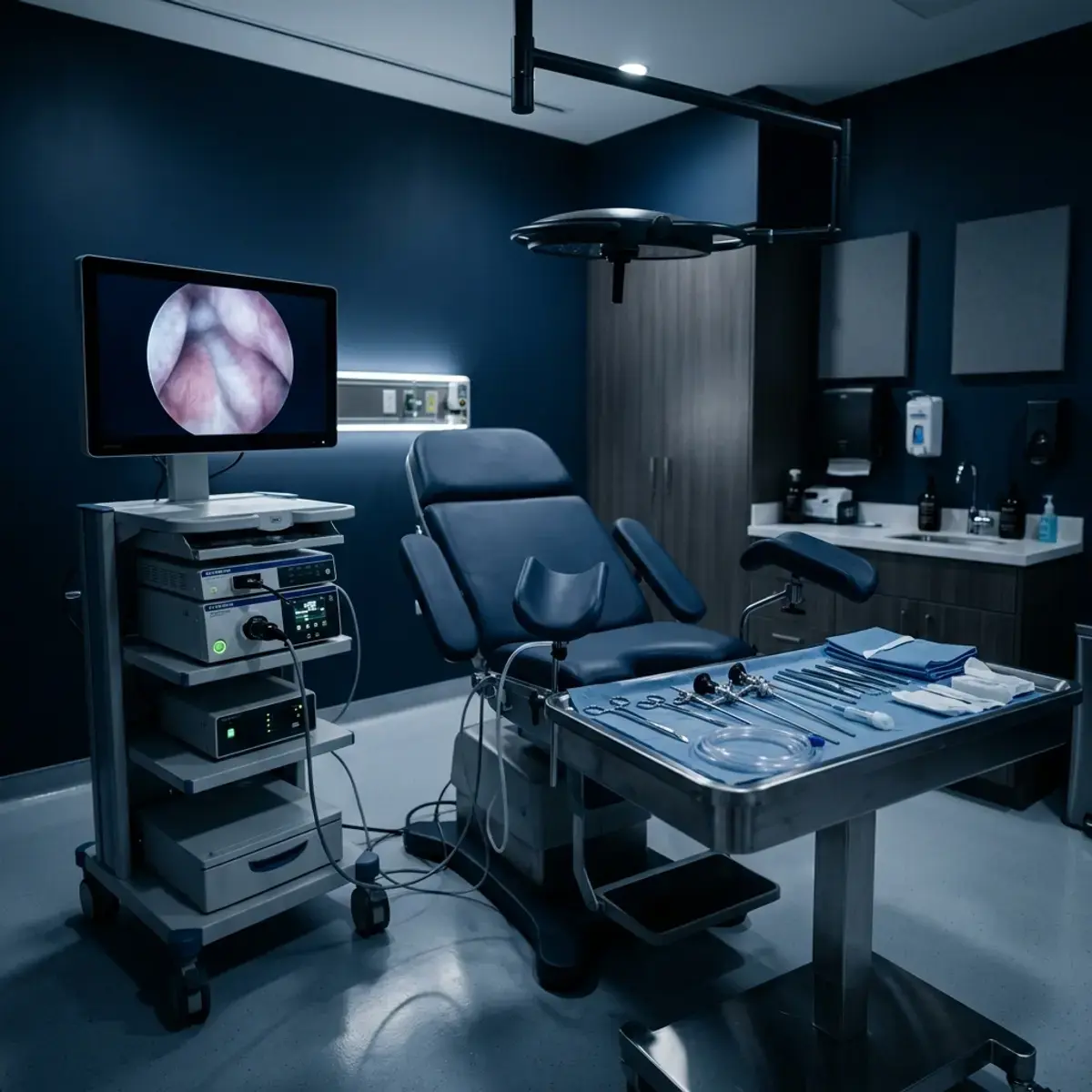
Hysteroscopy - Minihysteroscopy
Hysteroscopy is a minimally invasive diagnostic and therapeutic procedure that allows direct visualization of the uterine cavity using a thin optical camera. It is performed as an outpatient procedure, takes 15–30 minutes, usually without general anaesthesia, with same-day recovery.
What is hysteroscopy
Hysteroscopy represents the "gold standard" in the diagnosis and treatment of changes in the uterine cavity. It is a minimally invasive, short-term procedure that allows the gynecologist to inspect the uterine cavity in order to diagnose and treat causes of disorders and diseases of the uterus.
A hysteroscope is a thin endoscopic instrument (a micro camera with a source of cold light) that is inserted into the uterus and allows visualization of the uterine cavity. Palmotićeva Clinic is equipped with a modern Karl Storz hysteroscope that allows diagnostic and operative hysteroscopy with little or no dilation of the cervical canal.
Hysteroscopy is performed both for diagnostic purposes and for treatment:
- Diagnostic hysteroscopy (mini hysteroscopy) — provides the gynecologist with information necessary for accurate diagnosis: adhesions, endometrial polyps, fibroids, uterine cavity deformities, Asherman's syndrome
- Operative hysteroscopy — manipulations within the uterus where the doctor carefully removes causes of uterine disease: polypectomy, removal of adhesions and septa, targeted endometrial biopsy
When is hysteroscopy recommended
Hysteroscopy is recommended in the following cases:
- Unexplained forms of infertility and preparation for IVF
- Heavy or irregular uterine bleeding
- Suspected endometrial polyps or submucosal fibroids
- Adhesions (synechiae) preventing pregnancy
- Asherman's syndrome and uterine cavity deformities
- IUD embedded in the myometrium
- Unexplained pelvic pain
- Suspected premalignant and malignant uterine conditions
As a routine procedure, it should be performed in all patients before their first IVF cycle — this significantly reduces the number of unsuccessful cycles.
How the procedure works
Preparation:
- Refrain from eating and drinking for at least 6 hours before the procedure
- A clean vaginal and cervical swab result is required
- The doctor may request additional swabs for chlamydia, mycoplasma, and ureaplasma
- Best timing: first phase of the cycle (up to day 10 of menstruation)
During the procedure:
Hysteroscopy is performed on an outpatient basis — there is no overnight stay. Duration depends on whether it is diagnostic or operative: from 15 minutes to two hours including preparation and recovery.
Recovery:
Recovery is very quick. After the effect of anesthesia wears off, mild cramping in the lower abdomen may be felt. Most patients can freely return to their usual activities the next day.
Advantages of hysteroscopy
- No incisions — minimally invasive procedure
- Quick recovery — return to activities the next day
- High precision — direct visualization of the uterine cavity
- Diagnosis and treatment in a single procedure
- Avoids "blind" curettage — targeted approach
- Significantly increases chances of successful IVF
You can check the price of hysteroscopy in our price list.

Performed by
Dr Đorđe Petković
Consultant in Operative & Endoscopic Gynaecology · 17+ years of experience
Metode i Operacije
Odaberite specifičnu vrstu histeroskopske intervencije za detaljnije informacije o samom zahvatu.
Dijagnostička histeroskopija
Zlatni standard za mikroskopski pregled unutrašnjosti materice i rasvetljavanje uzroka steriliteta.
Histeroskopska polipektomija
Napredno uklanjanje polipa bez struganja zdravog zida radi maksimalnog očuvanja fertiliteta.
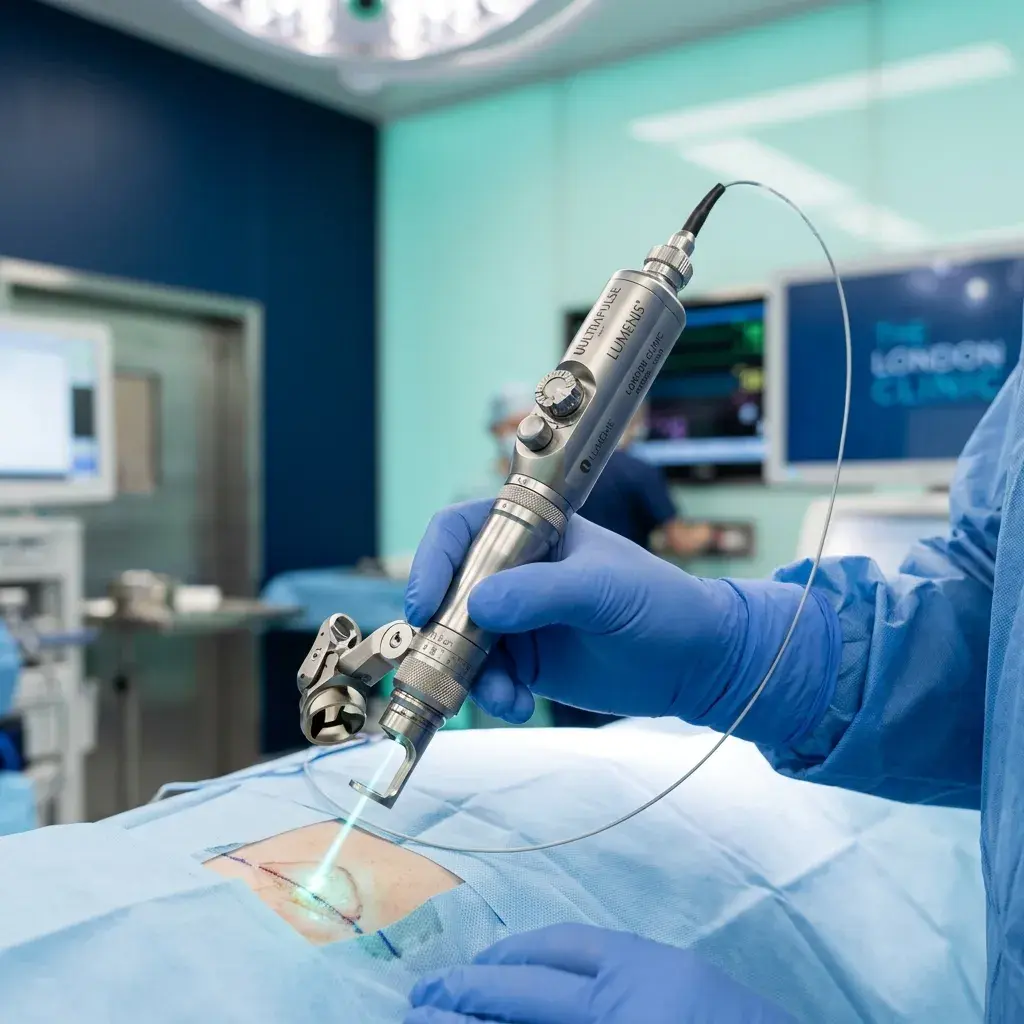
Histeroskopska miomektomija
Suptilno uklanjanje submukoznih mioma kamerom iz same šupljine, bez ikakvog agresivnog reza.
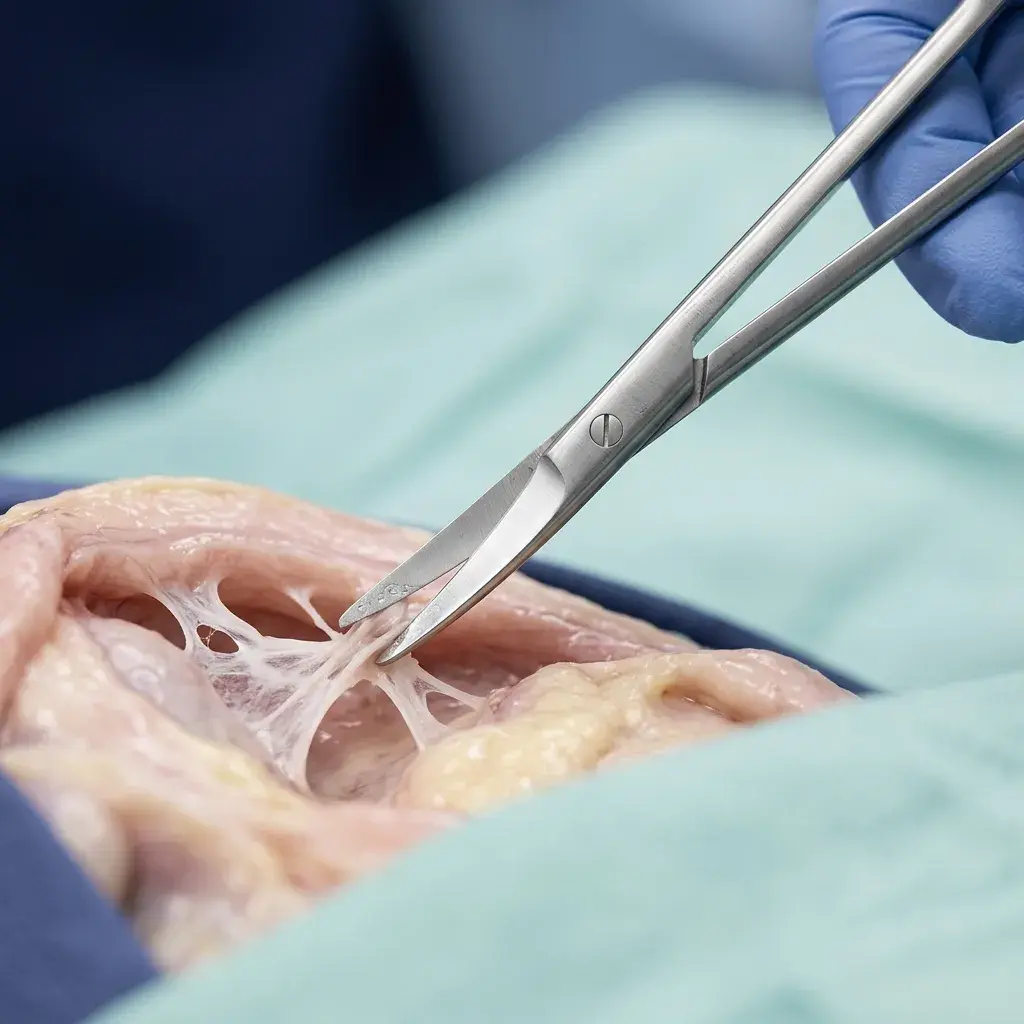
Otklanjanje sinehija
Mikroskopska tehnika rešavanja priraslica (Ašermanov sindrom) zarad uspostavljanja ciklusa.

Uklanjanje pregrade (Septum)
Histeroskopsko seciranje pregrade za optimalan oblik materice pre ulaska u VTO proceduru.
Patients often ask
Hysteroscopy is an examination of the inside of the uterus using a thin camera (hysteroscope) inserted through the cervix. The doctor views the uterine lining on a monitor and can immediately take biopsies or remove abnormalities. The procedure takes 15–30 minutes.
Diagnostic hysteroscopy is performed without or with local anaesthesia — most patients feel only mild discomfort. Operative hysteroscopy is done under brief general anaesthesia, so you feel nothing during the procedure.
Recovery is quick. After diagnostic hysteroscopy, a few hours of rest is sufficient. After operative hysteroscopy, you return to normal activities within 1–2 days. Mild bleeding or cramping may last up to 5 days.
Hysteroscopy is recommended for abnormal uterine bleeding, suspected polyps or fibroids, fertility problems, post-curettage assessment, investigating pelvic pain, and diagnosing Asherman syndrome.
Current prices for diagnostic and operative hysteroscopy are available on our price list page. The price includes the procedure, specialist consultation and report. For operative hysteroscopy, the cost depends on the scope — call us for exact information.
Preparation is minimal. Arrive on an empty stomach (6 hours without food), bring previous test results and avoid aspirin 7 days before the procedure. It is usually scheduled right after menstruation.
Hysteroscopy is a very safe procedure with an extremely low complication rate. Rare risks include mild bleeding or infection. Outpatient performance further reduces risk compared to hospital settings.